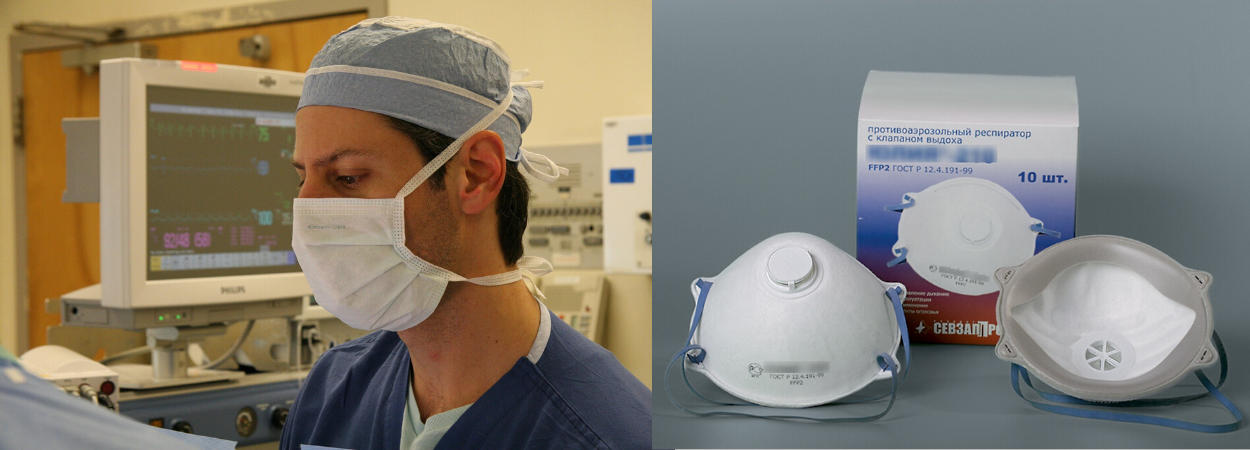
Left: A medical professional wearing an ordinary surgical face mask during an operation
Right: FFP2 Respirators designed to make a tight face seal
As the storms approached our shores from afar, many have instinctively rushed to purchase face masks and face respirators in a bid to stave off the dreaded coronavirus. However, some explanation is needed in order to clarify the confusion surrounding these simple face masks, and the not so simple face respirators.
A surgical face mask is designed to limit the amount of aerosols (finely divided droplet spray) that are emitted from a surgeon’s mouth and nose from contaminating the surgical field. They protect the patient from the surgeon, and not the surgeon from the patient. The mask material has pores many times larger than a virus and is not tight fitting to the face. Hence, they are not very effective at protecting the wearer from very fine dust, or indeed virus laden aerosols. They are however somewhat effective at preventing one from touching the nose and face with possibly contaminated hands.
Respirators are a completely different kettle of fish. They are much better fitting to the face and are meant to make a seal. They need to be fit tested and should be used together with other personal protective equipment (PPE), particularly eyewear for maximum effectiveness. Yet, what many might not be aware of, is that high performance respirators (such as those rated to the American NIOSH N95/N100, or the European EN149 FFP2/FFP3 standards), are actually “electrical devices” that work using the physics of electrostatics to attract and then trap the tiniest of particles inside their non-woven electret polypropylene filters.
Electret materials are dielectric materials that retain a semi-permanent electrical charge within them. As long as this electrical charge persists inside the material making up a face respirator, very small particles (down to a few 10’s of nanometres) are reliably lodged within the mask. This is what gives these respirators the prized 95% (or higher) filtration efficiency, without making it unduly difficult to breathe through. This makes them suitable for handling hazardous dusts and fibres (like lead or asbestos).
Both face masks and respirators may become contaminated after use and must not be touched. If touched, the hands must then be washed immediately and thoroughly. Removal and disposal also has to be performed very carefully, lest these masks and respirators may become themselves a source of infection.
In times of shortages the temptation arises for reusing such disposable masks/respirators more than once. Since these could have been contaminated, reuse is highly inadvisable. Research suggests that it may take many hours, possibly several days for viable virus concentrations to drop sufficiently to make used masks safe to handle or reuse.
Moreover, washing a high performance respirator with alcohol (ethanol or IPA), water, detergent, or bleach damages these respirators irreversibly, by discharging the electret that makes them work. Autoclaving and other forms of heating also damages them. Medical practitioners in particular, should be especially careful.
An experimental technique involving intense short-wavelength (253 nm), germicidal ultraviolet radiation (UV-C) shows promise for sterilisation with minimal mask damage, and has been researched by several groups around the world. This is currently being evaluated at the University of Malta to mitigate the severe shortages of high performance respirators, particularly for medical professionals.
By Dr Ing. Marc Anthony Azzopardi, a lecturer with the Department of Electronic Systems Engineering